Uncovering Allergy Testing Part 2: IgE and You
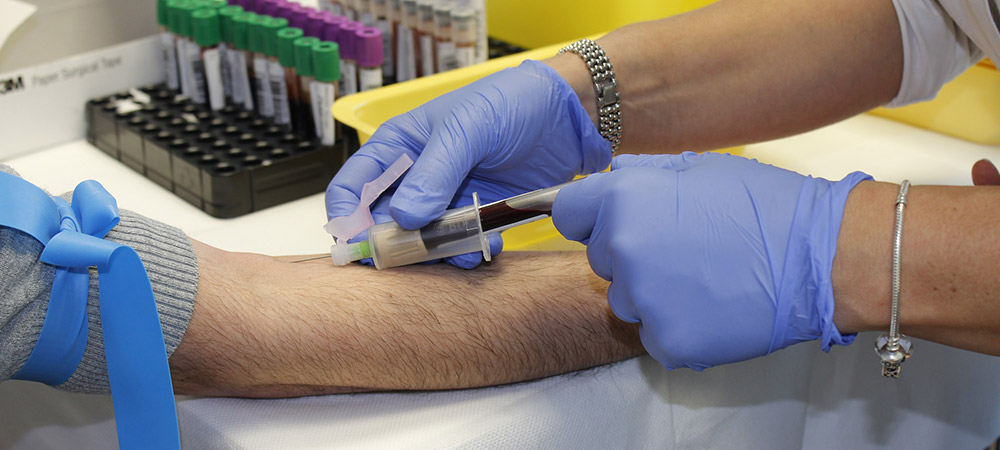
In our previous blog, we introduced the concept of blood testing (see Uncovering Allergy Testing Part 1: What Tests do I Need?). Before learning more about blood testing, I thought it was something that could easily be discussed in one paragraph, but, I was definitely wrong. It turns out blood testing is more complicated than it seems on the surface, and so is IgE. Already confused? Hang tight!
What is IgE?
To understand blood testing, you have to first understand IgE (immunoglobulin) — an antibody. When you are exposed to something you are allergic to, your immune system reacts and creates IgE to that particular item. The antibody travels and attaches to certain cells in your body, usually in the lungs, skin, or respiratory tract. The antibody “coats” the outside of the cell. When the allergen contacts the antibody on the cell wall, the cell wall is “tickled” and allergy hormones are released from the cell, which starts an allergy chain reaction.
Some people make IgE to specific items — one patient may make IgE to cat and therefore be “cat allergic” while another person may NOT make antibody to cat, but make it to dust mite and be “dust allergic.”
Dr. Mary Morris, a partner at Allergy Associates of La Crosse and author of the La Crosse Method™ Protocol, states, “Surprisingly, it’s only been since 1967 that we even knew about IgE antibodies. Skin testing has been done for 100 years, but blood testing really is more recent.”
How does blood testing work?
To understand how an individual person reacts to an allergen, drawing blood and taking a microscopic look at IgE is often done. The blood draw itself is like any other draw, but how the blood is examined is quite different.
In this test, the blood sample is exposed to an extract of a potentially offending allergen, for example, dust mite. If the blood contains IgE to dust mite, the two substances will bind together and stay attached. An enzyme is then added, which may cause the reaction to change color. If the sample changes color, the lab can determine the amount of IgE present in order to determine how allergic a person is to the antigen.
Dr. Morris explains that this has to be done for each potentially threatening allergen. “Each individual thing that we order — dust mite, ragweed pollen, grass, cat, dog — each has a different specimen well with this purified extract. Then the blood is added and each of those items gives us a separate test result.”
Understanding the numbers
Though the testing is elaborate, results are typically marked simply as having a positive IgE or negative IgE. Dr. Morris says, “The higher the number, the more of those allergy antibodies are present, and the more likely it is that the reaction is clinically significant.”
Positive IgE demonstrates that the immune system is producing the allergy antibody — the patient is sensitized. It’s important to know that a mildly positive result indicates sensitization, but not necessarily allergy. “Sensitization” means the presence of IgE in the absence of symptoms. “Allergy” is determined with a positive IgE in the presence of a convincing history of reactivity to the item. In essence, the blood test is determining the presence or absence of IgE. The doctor (with this test) determines whether the patient is “allergic.”
Negative IgE means that IgE is absent in the blood testing — the patient is likely not allergic. Interestingly, though, IgE can sometimes be produced near allergy cells in the skin, eyes, nose, lung, nervous system or gastrointestinal tract, and then may not travel through the blood in significant numbers. Therefore, sometimes IgE may be negative, or low, on a blood test, but a person may still be allergic. Since the blood test is measuring “free floating” IgE in the bloodstream and not the actual IgE affixed to allergy cells, the test is one step back from where the actual reaction is taking place. This is when skin testing may be beneficial, since it is injecting a potential antigen into a site of potential allergy cells (i.e., the skin).
As you can tell, the blood test results can be complicated, so making sure results match up with history is imperative to determine final results. Dr. Morris states, “History is number one. If the history matches up with the IgE level, we’re great. If it doesn’t, then we have to explore further.”
What goes up, must come down — or does it?
Once the allergen is detected, allergy drops work to train the immune system to not react — or to “not send out” those IgE antibodies. Patients are usually retested around three months after starting allergy drops, and most would expect their new IgE number would be less than when they were first tested. This is not always the case. Generally, the number will first increase.
When taking allergy drop immunotherapy using the La Crosse Method Protocol, patients are exposing themselves to the allergen multiple times a day and because of that, the specific IgE number may increase first before decreasing in the long run. This phenomenon has been well studied and does not indicate a worsening allergy. The mechanism causing the increased IgE in the blood is very different in the untreated individual compared to the treated patient. By the next visit, the numbers should generally decrease and symptoms should lessen.
You can also learn more about how sublingual immunotherapy works to alter IgE numbers.